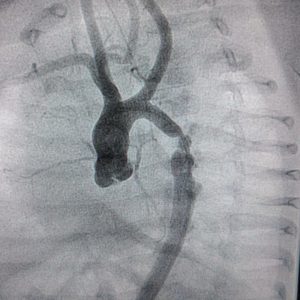
Background
Interventional radiology and interventional cardiology are increasingly used in children as minimally invasive procedures that can replace more complex pediatric surgical options. When fluoroscopy-guided interventional radiology and interventional cardiology procedures are performed in children, radiation doses can be relatively high and can cause reactions in tissue, such as skin lesions. For a given radiation dose, children generally have a higher risk of tumor induction than adults. It is estimated that the risk of radiation-induced cancer in people exposed in childhood may be between 2 to 3 times higher than an average population.
New technologies and post-processing of images for interventional radiology and cardiology allow a reduction in doses for the patient and medical personnel, while maintaining or improving image quality. This provides the opportunity to optimize these procedures if such technologies are implemented with the appropriate training in radiation protection and if a periodic audit of patient doses and image quality is carried out. The number of interventional procedures in pediatrics is increasing, especially in interventional cardiology, and in these cases, reducing the dose to the patient is a priority.
The International Basic Safety Standards (BSS), PAHO Resolution CSP28.R5, include specific requirements for medical exposures to patients and pay special attention to pediatric patients. The Bonn “Call to Action”, also includes recommendations aligned with those requirements, and the International Commission on Radiological (ICRP) has issued in 2017, new recommendations on Diagnostic Reference Levels (DRL), including tips for interventions and pediatrics. Only a few countries in the world have implemented the use of DRLs in pediatric interventional radiology and this project attempts to improve optimization using DRLs for these practices in Latin America and the Caribbean.